“But the Waiting Room is Empty!” – What Your GP Is Really Doing
You call your local surgery hoping for an appointment, only to be told there’s a wait. Or perhaps you walk past and notice the waiting room is empty. “How busy can they be?” you wonder. “Why can’t someone just see me now?”
Table Of Content
It’s a fair question. On the surface, general practice can look quiet. But that calm exterior hides an enormous amount of work happening behind the scenes – essential, complex work that remains invisible to patients. Let’s take a look behind the consulting room door and discover what your GP and the wider practice team are really doing.
The Work You Don’t See
Modern general practice extends far beyond face-to-face appointments. The traditional image of a GP seeing patients every 10 minutes for eight hours straight is now outdated.
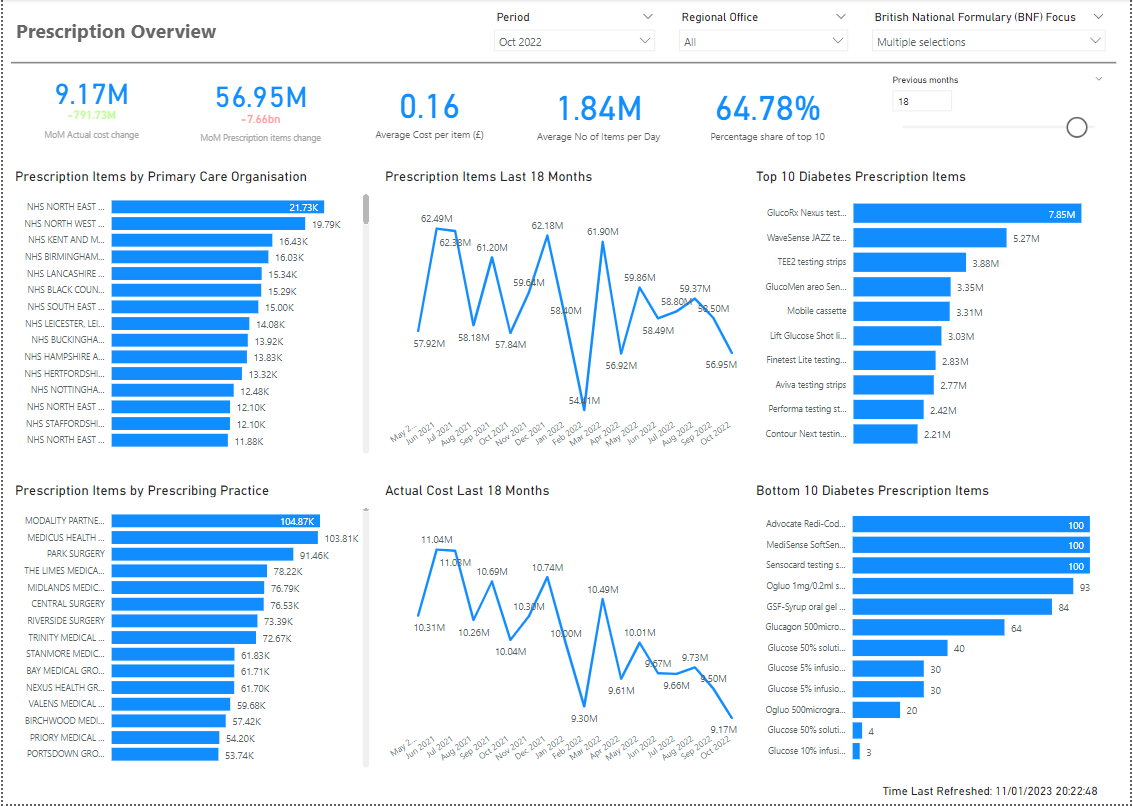
Today, GPs spend much of their time handling clinical tasks that never involve a waiting room – yet these tasks are crucial for your safety and care. A single practice might process up to 300 prescription requests daily. Each one requires careful review: Is the dose correct? Has the patient completed their monitoring tests? Do any recent hospital letters suggest changes? This involves clinical decision-making – not simple box-ticking – and it takes significant time.
Then there are test results from blood work, scans, and other investigations that need reviewing, interpreting, and sometimes require same-day action. A GP might dedicate their entire morning to working through results and calling patients to discuss next steps – or often, making multiple attempts to reach patients who don’t answer their phones.
And that’s just the beginning.
Phone Calls, Referrals, and Follow-Up
GPs make numerous outgoing calls daily – following up with patients, discussing new symptoms, explaining results, or checking in on vulnerable individuals. When patients don’t answer, this turns into repeat calls, voicemails, or letters. What appears to be a quiet desk often conceals a long list of names and numbers requiring attention – with important clinical decisions hanging in the balance.
Referrals to secondary care add another layer of work. When a GP determines a patient needs to see a hospital consultant or specialist service, the referral process isn’t instantaneous. Most referrals must be dictated, summarised, and submitted through structured systems – often requiring supporting documentation and precise clinical coding. This represents additional work that extends far beyond the initial appointment.
Caring Beyond the Consultation
Some patients require ongoing, frequent support – individuals sometimes referred to as high-intensity users. They may have multiple chronic conditions, mental health challenges, or complex social care needs. Their care doesn’t always involve surgery visits but demands regular reviews, coordination, and often urgent decision-making.
To support these patients effectively, GPs participate in regular multi-disciplinary team (MDT) meetings, collaborating with district nurses, social workers, mental health professionals, and others to ensure coordinated care. These meetings are essential for safeguarding, end-of-life care, dementia support, and more. This represents one of the most collaborative – and least visible – aspects of a GP’s week.
The Role of the Wider Team
GPs aren’t the only ones shouldering this workload. Behind every efficiently-run surgery stands a Practice Manager juggling everything from HR and finance to IT systems, compliance, building maintenance, complaint resolution, and staff wellbeing. They provide the essential foundation that keeps practices functioning – a role that has grown increasingly complex in recent years.
Many Practice Managers belong to the Institute of General Practice Management (IGPM), which works to amplify their voices nationally, raise awareness of their responsibilities, and advocate for the recognition they deserve. Without strong leadership at this level, practices would struggle to meet the demands of modern healthcare.
We shouldn’t overlook the contributions of reception teams, secretaries, prescription clerks, and nursing staff, all working diligently behind the scenes to maintain operations – answering phones, updating records, preparing referrals, coordinating with hospitals, and ensuring patients receive appropriate care when they need it.
Finding the Silver Lining
Yes, general practice faces significant challenges. Demand has reached unprecedented levels, and the sheer volume of work can be overwhelming. However, there are positive developments too.
Technology has enabled practices to manage care in innovative ways – from online consultations to remote monitoring of chronic conditions. Patients can now receive advice without always needing in-person visits. Staff are developing new approaches to triage and prioritise care, ensuring the most urgent needs receive prompt attention. Many practices share a genuine team spirit – a collective commitment to improving care, even under difficult circumstances.
The shift toward team-based care, with more clinical pharmacists, first-contact physiotherapists, and mental health practitioners working in practices, helps distribute the workload. GPs remain central to this system, but they’re no longer alone – benefiting both patients and healthcare providers alike.
So Why Does the Waiting Room Look So Quiet?
Because the real waiting room isn’t the physical space with chairs and magazines. It’s the digital queue – filled with lab results, prescription requests, incoming hospital correspondence, and patients awaiting callbacks. It’s the MDT meeting happening down the hall, or the GP at their desk writing a potentially life-saving referral.
When you’re told there’s a wait to see your GP, or you notice an empty waiting room, remember this: general practice hasn’t stopped working. It’s operating in less visible but equally vital ways.
Your GP isn’t sitting idle. They’re behind the scenes – reviewing, prescribing, calling, referring, consulting, and coordinating – often simultaneously. The quiet waiting room doesn’t indicate inactivity; rather, it reflects everything happening at once, just beyond your view.